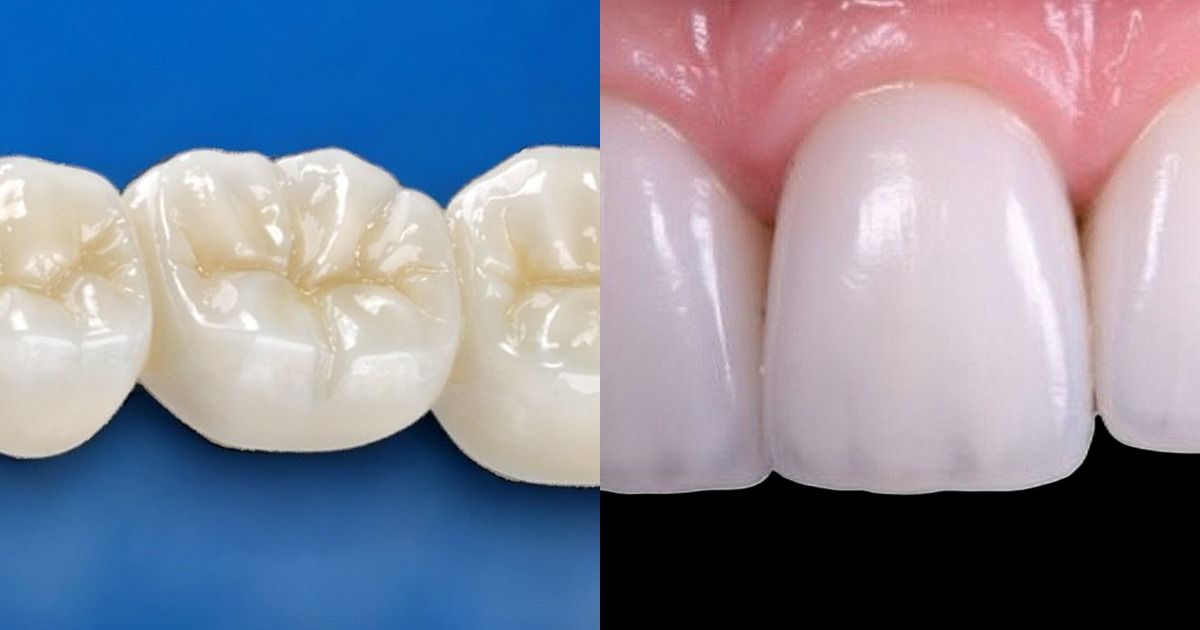
Multi-Layer Zirconia vs. Porcelain Layered Zirconia: Strength, Esthetics, and When to Use Each
When an anterior case needs both natural translucency and long-term durability, the decision often narrows to two zirconia-based options: multi-layer zirconia or porcelain layered zirconia. They share the same high-strength foundation and target the same esthetic zone, but they take fundamentally different paths to get there. One is a monolithic crown with built-in gradient translucency milled from a single blank. The other is a bilayer restoration with hand-layered ceramic that gives a ceramist full control over shade, depth, and characterization.
Each approach carries tradeoffs in strength, chipping risk, and esthetic ceiling that directly affect case outcomes and remake rates. This guide breaks down the clinical differences so you can match the right material strategy to the case, not default to the one you ordered last time.
The Short Version
Choose multi-layer zirconia
for cases that need a reliable blend of esthetics and durability without veneer chipping risk: premolars in the smile line, bruxism-prone patients needing anterior work, and situations where a monolithic solution simplifies the workflow.
Choose porcelain layered zirconia
when maximum esthetic control is the priority: high-visibility anterior cases, shade-matching challenges next to natural teeth, and patients who demand the most lifelike result and have favorable occlusal conditions.
How Each Material Achieves Esthetics
Multi-layer zirconia and porcelain layered zirconia start from the same base material but diverge sharply in how they deliver a natural appearance.
Multi-Layer Zirconia: Engineered Gradient
Multi-layer zirconia blanks contain multiple vertical zones of different yttria content within a single disc. The cervical region uses 3Y-TZP (3 mol% yttria), which is strong and more opaque. Moving toward the incisal, the composition transitions through 4Y-TZP to 5Y-TZP, progressively increasing the cubic crystal phase and improving translucency. The result is a monolithic crown with a built-in gradient: denser where it meets the margin, more translucent at the incisal edge. Because the entire restoration is milled from one block, there is no veneer interface to chip or delaminate. External staining and glazing provide the final shade characterization.
Porcelain Layered Zirconia: Handcrafted Depth
Porcelain layered zirconia takes a different path. A high-strength 3Y-TZP zirconia framework is milled first, then a skilled ceramist hand-layers compatible veneering porcelain over the framework. This layering process builds in fluorescence, opalescence, incisal halos, and the kind of nuanced surface texture that no milling algorithm currently replicates on its own.
For cases where fluorescence, opalescence, and fine-grained surface texture are the priority, hand-layered porcelain has historically represented the higher esthetic ceiling. A talented ceramist working with layered porcelain can produce restorations that closely mimic natural teeth. The tradeoff is that every advantage of that porcelain layer comes with the mechanical limitations of that porcelain layer.
Strength, Chipping Risk, and the Monolithic Advantage
Mechanical performance is where these two approaches diverge most sharply, and it is the factor most likely to influence your material choice on a case-by-case basis.
The numbers tell an interesting story. A porcelain layered restoration’s zirconia framework is just as strong as a monolithic zirconia crown, and that framework rarely fractures. The weak link is the veneering porcelain, which has a flexural strength of only about 60 to 120 MPa depending on the product, on the order of one-tenth of the substructure strength it sits on.
Multi-layer blanks, by contrast, maintain zirconia-level strength throughout the entire restoration. Even the most translucent incisal zone (5Y-PSZ) delivers flexural strength values in the range of roughly 470 to 650 MPa across major strength-gradient products, drawing on peer-reviewed measurements (Inokoshi et al., 2023; Strasser et al., 2023) and manufacturer specifications for leading product lines. This is comparable to lithium disilicate and far stronger than any veneering porcelain.
The Chipping Problem
Veneer chipping has been the most documented technical complication of porcelain layered zirconia restorations since the material’s introduction. A systematic review of implant-supported all-ceramic single crowns by Pjetursson et al. (2021) found that veneered designs had significantly higher annual ceramic chipping rates (1.65%) than monolithic designs (0.39%, p = 0.017). For tooth-supported single crowns, Sailer et al. (2015) and the updated systematic review by Pjetursson et al. (2026) report accumulated 5-year chipping rates in the low single digits for veneered zirconia. The rates climb higher for multi-unit fixed dental prostheses (FDPs), where Pjetursson et al. (2015) reported 5-year ceramic complication rates in the 10 to 15 percent range for densely sintered zirconia.
A more recent meta-analysis of tooth-supported multi-unit FDPs by Romandini et al. (2026) found that ceramic surface chipping was least frequent in monolithic zirconia designs, though 5-year survival was numerically similar across veneered (92.9%) and monolithic (87.9%) zirconia. The chipping advantage of monolithic does not automatically translate to a survival advantage.
Several factors drive this chipping risk: coefficient-of-thermal-expansion mismatch between zirconia framework and veneer, thermal residual stresses from cooling after porcelain firing (exacerbated by zirconia’s low thermal diffusivity), the low fracture toughness of veneering porcelain at occlusal contact points, inadequate anatomical support when framework design leaves unsupported porcelain, and layering technique (hand-layered porcelain shows higher chipping rates than pressed ceramics in systematic review data).
Multi-layer zirconia largely sidesteps this failure mode. Because there is no veneer interface, the delamination and thermal-mismatch problems that drive bilayer chipping are absent. Strength-gradient blanks do deliver somewhat lower composite strength than single-yttria 3Y monolithic zirconia, but the dominant mechanism is the intrinsic weakness of the higher-yttria 4Y and 5Y zones themselves (reduced transformation toughening, higher cubic fraction, larger grain size) rather than the inter-zone transitions. For the comparison with other monolithic and bilayer materials, Summit-Horizon’s guide to full contour zirconia vs. IPS e.max covers the broader material selection landscape.
Translucency and Esthetic Limits
If multi-layer zirconia solves the chipping problem, you might wonder why anyone still orders porcelain layered restorations. The answer is esthetic control.
Hand-layered porcelain gives the ceramist direct control over internal color effects that a monolithic block cannot replicate. Opalescence, fluorescence under UV light, incisal halos, maverick color effects, and surface texture that catches light the way enamel does. These details separate a restoration that looks like a tooth from one that looks like a very good crown.
Multi-layer zirconia has made significant strides. The gradient translucency built into modern blanks produces a natural cervical-to-incisal transition, and external staining adds shade customization. For premolars, lower anteriors, and many upper anteriors, the result is clinically excellent.
The gap has not closed entirely. A maxillary central incisor adjacent to a highly translucent natural tooth, a case with visible margins and thin tissue, a patient with unusually high esthetic expectations: these remain situations where porcelain layered zirconia justifies its added complexity.
Preparation Requirements
Prep design differences between these two options reflect the space each material system needs to function.
Multi-layer zirconia, being monolithic, requires reduction similar to standard full contour zirconia: typically 1.0 to 1.5 mm of occlusal clearance and 0.8 to 1.0 mm on axial walls. Chamfer or rounded shoulder margins work well. Because there is no veneer to accommodate, reduction can be slightly more conservative than a porcelain layered restoration, particularly in the incisal third.
Porcelain layered zirconia demands more room. Ivoclar's IPS e.max ZirCAD Clinical Guide calls for 1.5 to 2.0 mm of incisal reduction for bilayer anterior crowns, with a 1.0 to 1.5 mm minimum for the labial surface. Achieving the best esthetic result with full porcelain layering typically calls for somewhat more labial clearance, approximately 1.3 to 1.8 mm, to accommodate a zirconia framework of roughly 0.5 to 0.7 mm plus veneering porcelain of approximately 0.8 to 1.1 mm. Shoulder or deep chamfer margins are preferred. Inadequate reduction is one of the most common contributors to veneer fracture: when the lab must thin the porcelain or the framework to compensate for limited space, mechanical reliability drops.
Clinical Decision Guide: When to Use Which
Premolars and canines in the smile line where esthetics matter but chipping risk needs to stay low. Anterior cases in patients with known or suspected bruxism where the 5Y incisal zone is acceptable (for severe bruxers, full-contour 3Y zirconia remains the strongest option). Situations where a monolithic workflow reduces turnaround time and cost. Cases where the patient’s occlusion involves heavy anterior contact or edge-to-edge relationships. Long-span anterior bridges where veneer chipping risk accumulates across multiple units. Any case where the clinician values predictability over the highest possible esthetic ceiling.
Maxillary central and lateral incisors in high-visibility smile zones. Cases adjacent to highly translucent natural teeth where a monolithic crown might appear flat or opaque by comparison. Patients with elevated esthetic expectations who understand the maintenance tradeoffs. Single-unit restorations where the chipping risk is lower than in multi-unit spans. Situations where fluorescence, opalescence, and incisal characterization are clinically essential.
At Summit-Horizon, our multi-layer zirconia crowns are fabricated from gradient-translucency blanks using CAD/CAM milling, with external staining and glazing customized to each case. For cases that call for hand-layered porcelain, our porcelain layered zirconia restorations are built on high-strength 3Y-TZP frameworks with ceramic applied by experienced technicians who control every layer of color and translucency.
When a case sits in the gray zone, our team reviews the scan data, evaluates the opposing dentition, and discusses the options with you before fabrication begins. That collaborative planning is part of how Summit-Horizon operates as an extension of your clinical team.
Side-by-Side Comparison
| Factor | Multi-Layer Zirconia | Porcelain Layered Zirconia |
|---|---|---|
| Construction | Monolithic; milled from one gradient blank | Bilayer; zirconia framework + hand-layered porcelain |
| Flexural strength | 500–1,200+ MPa (varies by zone) | Framework: 900–1,200 MPa; veneer: ~60–120 MPa |
| Translucency | Good to very good; built-in gradient from 3Y to 5Y | Excellent; hand-layered porcelain provides maximum esthetic control |
| Chipping/delamination risk | Minimal; no veneer interface | Higher; veneer porcelain is the known weak point |
| Incisal reduction | 1.0–1.5 mm | 1.5–2.0 mm (framework + porcelain thickness) |
| Labial reduction | 0.8–1.0 mm | 1.3–1.8 mm |
| Margin type | Chamfer or rounded shoulder | Shoulder or deep chamfer |
| Esthetic customization | External staining and glazing after milling | Full internal layering: fluorescence, opalescence, incisal halos |
| Best zone | Premolars, canines, and many anterior cases | High-visibility anterior: maxillary centrals and laterals |
| Bruxism suitability | Good; monolithic design resists parafunctional forces | Poor; veneer layer is vulnerable under heavy occlusal loads |
| Multi-unit bridge suitability | Yes; chipping risk does not accumulate across units | Use with caution; chipping rates increase in multi-unit FDPs |
| Relative cost | Moderate | Higher; hand-layering adds labor and time |
Frequently Asked Questions
Can multi-layer zirconia really match the esthetics of hand-layered porcelain?
For most clinical situations, yes. Modern multi-layer blanks with 4Y and 5Y incisal zones produce natural translucency gradients that satisfy the majority of patients and clinicians. Where multi-layer falls short is in extreme close-up esthetic demands: matching a single central incisor next to a highly translucent natural tooth, or reproducing specific internal color effects like opalescence and incisal halos.
How significant is the chipping risk with porcelain layered zirconia?
It is the most commonly reported technical complication for veneered zirconia restorations. A systematic review of implant-supported all-ceramic single crowns documented an annual ceramic chipping rate of 1.65% for veneered designs versus 0.39% for monolithic (Pjetursson et al., 2021). Tooth-supported veneered zirconia single crowns show accumulated 5-year chipping rates in the low single digits (Sailer et al., 2015; Pjetursson et al., 2026), and cumulative 5-year rates climb into the 10 to 15 percent range in multi-unit FDPs (Pjetursson et al., 2015). Most chipping events are minor and repairable (Heintze & Rousson grades 1-2), but some expose the framework and require full replacement. Proper framework design and appropriate case selection reduce the risk.
Should I avoid porcelain layered zirconia in bruxism patients?
In most cases, yes. Patients with documented bruxism or suspected parafunctional habits generate forces that exceed the mechanical tolerance of veneering porcelain. Multi-layer zirconia, full contour zirconia, or high-translucency zirconia are safer choices for these patients. If a bruxism patient requires the highest esthetic result and porcelain layered zirconia is selected, a custom nightguard should be part of the treatment plan.
What is the difference between multi-layer zirconia and high-translucency (HT) zirconia?
High-translucency zirconia is typically milled from a single-composition blank (often 5Y-PSZ) that prioritizes light transmission throughout the entire restoration. Multi-layer zirconia uses a gradient blank that transitions from high-strength 3Y-TZP at the cervical to high-translucency 5Y-PSZ at the incisal. The multi-layer approach provides better strength at the margin while still delivering translucency where it matters most. HT zirconia may offer slightly better overall translucency but at the cost of reduced strength in the cervical region.
How does Summit-Horizon decide which material to recommend?
Our team evaluates the digital scan, opposing dentition, occlusal scheme, and any clinical notes you include with the case. If the situation clearly favors one material, we proceed. Cases that fall in a gray area prompt a conversation before fabrication. Our goal is a restoration that seats right, looks right, and lasts, and that starts with putting the right material in the right case.
The choice between multi-layer and porcelain layered zirconia comes down to recognizing which tradeoff matters more for the specific case on your schedule. When mechanical predictability and resistance to chipping take priority, multi-layer zirconia delivers. For cases demanding the highest level of esthetic customization where occlusal conditions allow it, hand-layered porcelain is difficult to match.
Not sure whether multi-layer or porcelain layered zirconia is the right fit for your next anterior case? Contact Summit-Horizon to talk through the clinical situation with our team, or submit a case and we will review the scan data, evaluate the occlusion, and recommend the material approach most likely to deliver a confident result.
References
Share Post
Search Post
Recent Insights