How Surgical Guides Improve Implant Placement Accuracy and Reduce Chairside Adjustments
Without a surgical guide controlling the drill path, even a well-planned implant case can go sideways. The osteotomy drifts 2 mm lingual and 5 degrees off axis, the pre-designed abutment no longer seats passively, and the screw channel exits through the facial. Implant placement accuracy, or the lack of it, turns what should have been a confident first-time seat into a chairside adjustment session.
That scenario plays out more often than most clinicians would prefer. Freehand placement relies on the surgeon’s spatial interpretation of 2D imaging in a 3D surgical site, and even experienced operators produce meaningful deviations. Surgical guides close that gap by transferring a software-driven plan to the mouth through a 3D-printed template with embedded drill sleeves.
This post covers how guided surgery works, what the accuracy data shows, and why implant positioning matters as much to the prosthetic outcome as the surgical one.
The Short Version Digitally designed surgical guides reduce angular deviation by roughly half compared to freehand placement and produce more consistent apical and coronal positioning. Summit-Horizon merges your IOS and CBCT data, proposes a virtual implant position, and prints the guide on Asiga MAX or Asiga Pro 4K printers at micron-level resolution, so the implant lands where the prosthetic plan needs it.
What a Surgical Guide Actually Does
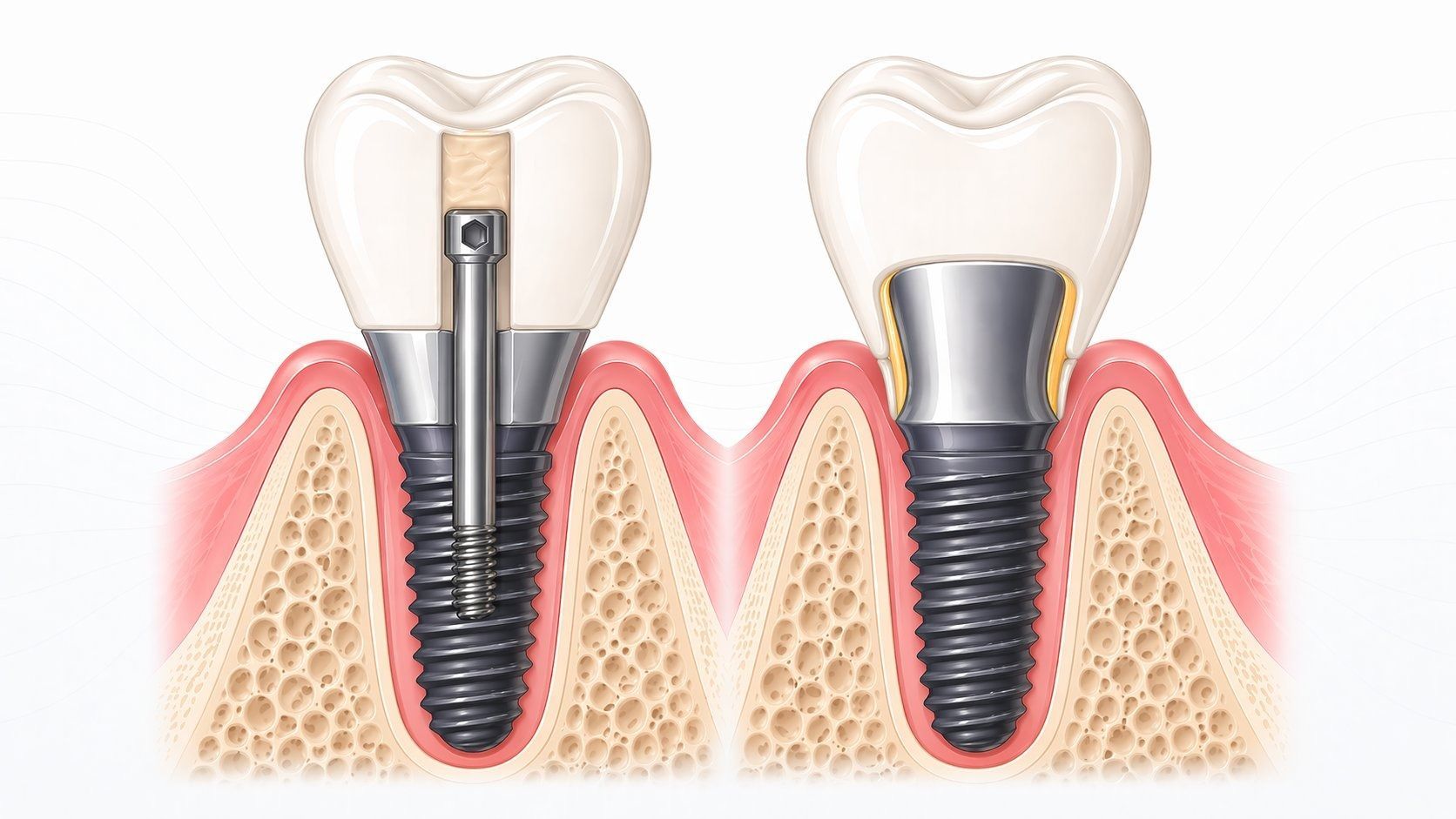
A surgical guide is a 3D-printed template that fits over the patient’s existing teeth, soft tissue, or bone and physically restricts the handpiece to a predetermined drilling path. Metal sleeves embedded in the guide control the position, angulation, and depth of each sequential drill in the osteotomy sequence. The implant itself can also be placed through the guide in a fully guided protocol.
Unlike freehand surgery, where the clinician mentally translates a 2D plan into 3D anatomy while managing access, visibility, and patient movement, a surgical guide removes much of that spatial interpretation. All critical decisions happen before surgery, during digital implant treatment planning , where the clinician can evaluate bone density, proximity to the inferior alveolar nerve or maxillary sinus, and prosthetic position in a merged 3D dataset. The guide simply transfers that plan to the mouth.
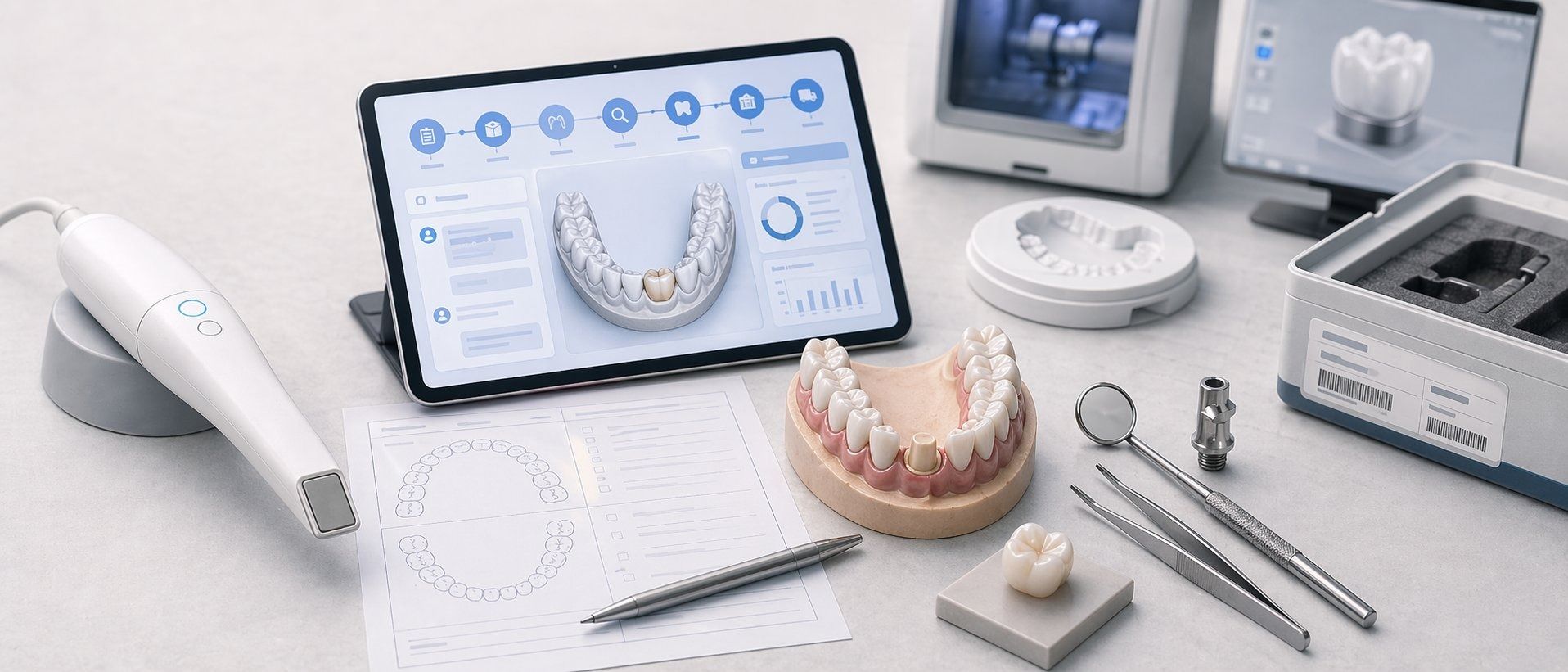
The Digital Planning Workflow: From Scan to Surgical Template
Guided surgery starts well before the patient sits in the chair. The workflow follows a defined sequence, and each step feeds the next.
Data Acquisition
The clinician captures an intraoral scan (IOS) of the arch and an opposing scan for occlusal registration. Separately, a cone-beam computed tomography (CBCT) scan provides the volumetric bone data. Summit-Horizon accepts scans from all major IOS platforms, including Primescan, Medit, iTero, and 3Shape TRIOS, in STL format.
Virtual Planning
Surface scan data and CBCT volume are merged in implant planning software. Summit-Horizon's design team works in 3Shape and DS InLab and supports clinician-led planning in SICAT Implant, CEREC Guide 3, and other major platforms. Within the merged dataset, the clinician and lab can collaboratively position the virtual implant with full visibility of bone volume, cortical thickness, nerve canals, sinus floor, and the planned prosthetic contour. Implant diameter, length, angulation, and depth are set with consideration for both the surgical anatomy and the restorative outcome.
Guide Design and Fabrication
Once the virtual implant position is approved, the software generates the guide geometry around it, incorporating drill sleeves at the exact planned trajectory. Summit-Horizon 3D prints the guide on Asiga MAX and Asiga Pro 4K printers, which operate at micron-level pixel resolution. After printing, the guide is inspected for fit accuracy, finished, and delivered ready for chairside sterilization.
What the Accuracy Data Shows
The clinical case for guided surgery rests on a growing body of evidence comparing guided and freehand implant placement across thousands of implants.
Freehand coronal deviation ~1.6 mm from Schnutenhaus et al., 2021; apical ~2.4 mm and angular range from Varga et al., 2020.
A landmark systematic review and meta-analysis by Tahmaseb et al. (2018), covering 20 clinical studies and 2,238 implants placed with static guides, reported mean deviations of 1.2 mm at the entry point, 1.4 mm at the apex, and 3.5° of angular deviation. Clinical studies of freehand placement, by contrast, report mean angular deviations ranging from 7° to over 10°, with substantially wider scatter in maximum values (Schnutenhaus et al., 2021; Varga et al., 2020).
More recent data reinforces these findings. A 2025 meta-analysis of 45 studies found that, pooling the 22 included clinical studies, computer-assisted workflows produced mean improvements of 0.65 mm in coronal deviation, 1.10 mm in apical deviation, and 3.87° in angular deviation compared to freehand placement, all statistically significant (P < 0.001). The 23 in vitro studies pooled separately showed smaller but directionally consistent improvements.
The consistency advantage matters as much as the mean numbers. Freehand placement shows a large range between best-case and worst-case outcomes. One clinical study recorded freehand angular deviations ranging from 0.71° to 21.30° across patients (Varga et al., 2020). Guided surgery compresses that range, producing more predictable results across cases and across operators.
Failure rates also differ by approach. A 2021 systematic review and meta-analysis reported guided placement failure at 2.25% versus 6.42% for freehand (Abdelhay et al., 2021).
Why Placement Accuracy Affects the Prosthetic Outcome
From a lab perspective, implant position is the foundation of everything that follows. The abutment design, screw channel emergence, contour of the final crown, and passive fit of multi-unit frameworks all depend on the implant landing where the plan says it should.
When an implant deviates significantly from the planned position, the prosthetic consequences cascade. A 5° angular deviation at the platform translates to roughly 1 mm of lateral displacement at the apex of a 12 mm implant (tan 5° × 12 mm ≈ 1.05 mm), and more for longer implants. That displacement can push the screw access channel through the facial surface of an anterior crown, force the use of an angled abutment that compromises the emergence profile, or create a cantilever load on a multi-unit bridge that was designed for axial loading.
For implant-supported restorations , the practical result is more chairside adjustments, longer appointments, and sometimes a remake. A screw-retained implant crown designed for a specific position cannot simply be modified to accommodate a different one. The abutment and crown may need to be re-fabricated entirely, adding turnaround time and cost for both the practice and the patient.
Guided surgery does not guarantee a perfect prosthetic outcome on its own. But placing the implant where the prosthetic plan expects it eliminates one of the most common sources of downstream complications.
When Guided Surgery Adds the Most Value
Implants are adjacent to critical anatomy such as the inferior alveolar nerve, mental foramen, or maxillary sinus floor. Immediate loading protocols require precise prosthetic position from day one. Full-arch cases demand parallel placement across four to six implants with controlled depth and spacing. Flapless approaches eliminate direct bone visualization, making the guide the only spatial reference. Limited interarch space or restricted mouth opening makes visual confirmation of drill angulation difficult. Bone volume is compromised and precise angulation is needed to engage available cortical bone while avoiding fenestration.
The benefits are not limited to complex cases. Single-tooth implants in the esthetic zone benefit from the positional predictability, especially when a screw-retained restoration with a palatal or lingual screw access is the goal. General practitioners who place implants regularly but want to reduce variability across their caseload also find guided protocols valuable. In vitro research on dynamic navigation suggests that navigation systems can reduce the performance gap between experienced and less-experienced operators in phantom models (Wang et al., 2023). Whether the effect size holds for static guides in clinical settings is still being studied.
Summit-Horizon’s Guided Surgery Workflow
Summit-Horizon supports guided surgery from digital planning through guide delivery. The workflow integrates with your existing scanner and follows a collaborative model: you provide the scan data, and our team handles the technical design and fabrication.
Planning begins when you submit your IOS scan and CBCT data through our digital implant planning workflow. Our team merges the datasets and proposes a virtual implant position based on your clinical notes, the available bone, and the planned restoration type. You review and approve the plan, or request modifications, before the guide goes to fabrication.
Guides are 3D-printed in-house on Asiga MAX and Asiga Pro 4K printers. The Asiga MAX delivers a 62-micron native pixel size, which supports accurate sleeve positioning. After printing, every guide is inspected for dimensional accuracy, proper sleeve seating, and fit on the model before shipping. Michael Wandling, MBA, Master CDT, contributed to the development of the CDT Digital Workflow specialty, and that expertise informs how our team approaches digital planning and guide fabrication.
Summit-Horizon also offers a training video library covering digital implant workflows, from scan capture through prosthetic delivery. If you are new to guided surgery or transitioning from freehand placement, these resources can help bridge the learning curve.
Limitations and Realistic Expectations
Surgical guides improve accuracy and consistency, but they do not eliminate deviation entirely. The Tahmaseb meta-analysis reported mean errors, not zero errors. Even with a well-designed guide, small discrepancies between planned and actual implant position will occur.
Several factors influence how closely the final result matches the plan. Guide fit is paramount: a guide that rocks or lifts off the supporting teeth or tissue during drilling introduces positional error at every step. Fixation screws reduce guide movement, especially for mucosa-supported designs in edentulous arches, where tissue compressibility is a concern. Guides in partially edentulous cases tend to show better accuracy than guides in fully edentulous cases (Tahmaseb et al., 2018).
Registration quality also matters. If the CBCT and IOS datasets are not accurately merged, the virtual plan itself carries an inherent offset that the guide faithfully reproduces. Using the same reference teeth for both scans and verifying the merge in software reduces this risk.
Finally, guided surgery does not replace clinical judgment. Bone density, soft tissue conditions, and intraoperative findings may require the clinician to modify the approach even with a guide in hand. The value of the guide is that it provides a precise starting point and a physical constraint, not that it makes decisions for the surgeon.
Planning an implant case that could benefit from guided surgery? Contact Summit-Horizon to discuss digital planning options with our team, or submit your IOS and CBCT data to get started. We will merge your scans, propose a virtual implant position, and fabricate a precision 3D-printed guide designed to put the implant exactly where your prosthetic plan needs it.
References
Share Post
Search Post
Recent Insights